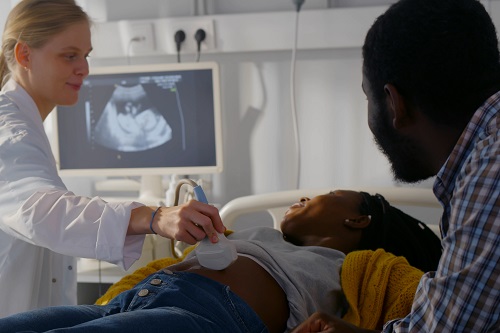
Experts outline recommendations for reducing traumatic birth experiences
February 14, 2024Implementation of these recommendations could potentially reduce traumatic births and improve outcomes for women and families...

The Centre for Maternal and Child Health Research carries out high quality research to improve the health and care of women, children, families and communities. The Centre provides an environment for the multi-disciplinary development of ideas and research initiatives in collaboration with professional, voluntary and service user organizations. The Centre has direct links with relevant professional educational programmes at City, University of London, such as midwifery, health visiting, public health and child nursing, which enable the rapid transfer of research into education and healthcare practice.
The Centre has three main research groups:
Cross-cutting themes are:

Research group lead: Professor Christine McCourt
Our research focuses on evaluating models of maternity, child and family services and care. Our work aims to improve care through rigorous studies using a range of methodologies with an emphasis on evidence-based care, appropriate uses of technology, service change and development and professional and user experience issues. This theme also has a strong inter-disciplinary thread of applying social science concepts and epidemiological approaches to clinical and organisational issues. Much of our work adopts a critical theory perspective and takes account of the complexity of healthcare interventions and contexts.
We are currently involved in a range of research projects and programmes on issues such as implementation of evidence based practice in maternity care, implementing NICE guidance on birth in different settings, factors influencing the uptake of midwifery units, trialling of home monitoring of blood pressure, development and trial of a group model of ante- and postnatal care – Pregnancy Circles (see projects), inter-professional relationships and retention in midwifery and health visiting (COPE study – see projects) and analysis of maternity outcomes by time of day and day of the week. Areas of interest within the group include concepts of choice, risk and safety and their relationship with service delivery and change, professionalisation processes and experiences, gender and healthcare and concepts of motherhood, childhood and the family. Our work is funded by a range of sources, including the National Institute for Health Research, the European Union and the Medical Research Council.
Our findings have been published in high impact journals and presented at conferences around the world. We have established links with a range of user, professional and policy organisations and university departments at local, national and international levels. Our work has influenced the development of maternity services throughout the United Kingdom (UK) and internationally, and has influenced health policy and guidelines in this area.
Sono-breech is a diagnostic accuracy study with the primary aim of finding out if midwives can accurately identify which way up a baby is before it is born using a small hand-held ultrasound device. The nested acceptability study, hosted by the SHPS Maternal and Child Health Research Centre, has been designed to explore possible barriers and facilitators for implementing this new technology into routine midwifery antenatal care.
Acceptability study lead and contact is Dr Mandie Scamell.
Sono-breech is a NIHR Health Technology Assessment project led by Imperial College London and supported by Cardiff's Centre for Trials Research: NIHR152029 - Diagnostic accuracy of handheld ultrasound at 36 weeks of gestation to determine fetal presentation.
The Research for Equitable Antenatal Care and Health (REACH) Pregnancy Circles study is the largest randomized controlled trial of group antenatal care undertaken internationally to date, and is the first to take place in the NHS. It aims to explore whether group antenatal care can improve the outcomes and the wellbeing of mothers and babies. Following a pause in trial recruitment due to the Covid-19 pandemic, the trial has now been extended until January 2024.
To find out more about the study, including how to participate please visit the REACH blog.
A number of City Masters and PhD students have worked with the REACH team and City has also developed training in group care facilitation for midwives both as stand-alone workshops and a Masters module.
Publications:
The NIHR funded SNAP2 programme, focused on self-management of blood pressure postnatally for women with high blood pressure, commenced in May 2022. It follows on the BUMP programme, which is now completed. The BUMP programme, also funded by the National Institute for Health Research and led by Professor Richard McManus at the University of Oxford, investigated whether giving pregnant women the means to monitor their own blood pressure and urine safely from home, in addition to the usual clinic monitoring, can result in an earlier diagnosis of raised blood pressure and pre-eclampsia. It also investigated the acceptability and practicality of this approach from women’s and professionals’ viewpoints and any impact on women’s experiences of their pregnancy. The trials found that self-monitoring was safe but did not lead to an improvement in clinic detection of blood pressure:
The linked qualitative studies found that pregnant women with higher risks of pre-eclampsia and professionals considered self-monitoring of blood pressure in pregnancy, in addition to usual care, acceptable and had the potential to enhance communication around care. Articles are currently in process.
MUSA provides a structured framework to guide the improvement of MUs in the UK and Europe, through a self-assessment tool and stakeholder engagement. It was developed from the Midwifery Unit Standards (accredited by NICE), in collaboration with international expert stakeholders. MUSA is the culmination of research and impact work that has been taking place at City, University of London since 2016 on the improvement and implementation strategies for scaling up the use of Midwifery Units.
The MUSA Toolkit offers a practical framework for the assessment and implementation of these standards, involving an improvement plan of high impact actions co-produced in partnership with key stakeholders. MUSA has been funded by research translation awards first to develop and test the toolkit (2020), to refine it through six case studies (2021) and to support its migration online (2022). We have successfully worked with several MUs across the UK and Europe to explore the impact of the MUSA Toolkit and are currently working on a regional implementation with the NHS in the North East of England.
Publications:
Cherish is a programme development project funded by the National Institute for Health Research to do the early work needed to co-design a personalised support package for improving outcomes for women and birthing people aiming for a spontaneous labour and birth. The Cherish team is made up of service-users, maternity improvement campaigners, midwives, obstetricians, statistician, and maternal health researchers and is led by Dr Mandie Scamell.
This evaluation project was commissioned by NHS England to provide a rapid independent evaluation of the implementation of this national maternity service priority. Led by Dr Ellinor Olander and Professor Christine McCourt, the team have conducted a national online survey of implementation leads and follow-up interviews with a sample, plus three rapid-enquiry case studies of maternity services with differing experiences of implementation. A link will be provided here to the evaluation report when this is published.
The aim of this project is to enhance collaboration amongst healthcare professionals delivering care for women and their families during and after pregnancy.
The current way of obtaining consent for this procedure, which is commonly done awake, is outdated. It can leave patients disempowered, worried, confused and with wrong expectations. Legal specialists in the field of gynaecology have suggested the use of consent aids co-developed with users. Honorary reader Dr Liza Ball and research fellow Dr Rose Coates have obtained funding from Barts Charity, backing from the Royal College of Obstetrician and gynaecologists and ethical approval to develop a video as a consent aid for outpatient hysteroscopy. A virtual workshop was organised and experience of this will be shared in an upcoming research seminar.
Euro-Peristat is a collaboration between the 27 members of the European Union plus Iceland, Switzerland, Norway and the United Kingdom. Although these countries share similar standards of living and health care, they vary considerably in their health policies and healthcare practices. Comparisons between them are therefore useful for raising questions about the implications of these differences. The project is coordinated by Jennifer Zeitlin of INSERM in Paris. Professor Alison Macfarlane is responsible for liaising between the countries of the UK.
The report published in November 2022 was its fifth. Like its predecessors, it aims to present data derived on a comparable basis for nine of its ten core statistical indicators. It was the first to present annual rather than five yearly data, using new improved methods described in the report. It presents data for the five years 2015 to 2019, as a baseline for the data for the pandemic year 2020 which will be published in 2023.
Because relatively few data are compiled for the UK as a whole, the report also contains data for Scotland, Northern Ireland, England and Wales combined and Wales separately. The report plus press releases issued centrally and by individual countries, plus journal articles and earlier reports can be found on the project web site:
This study looked at variations in the outcome of pregnancy by time of day, day of the week and season. It was funded by ESRC's Secondary Data Analysis Initiative and built on previous research which investigated the timing of births in England and Wales from 2005 to 2014. It linked administrative data about births linked to deaths in England and Wales in these years to hospital data about the care given at birth and data about subsequent admissions of mothers and babies to hospital.
Over 6 million births in England were included in an analysis of neonatal mortality by time of day and day of birth. Using a large dataset meant that data could be subdivided by onset of labour and mode of birth. It found that for spontaneous births and instrumental births and found there were no differences in mortality attributed to asphyxia, anoxia or trauma outside of working hours compared with working hours. Births by caesarean section were stratified by onset of labour and also showed no differences by timing of birth. A very small group of births, just two per cent of the total, were coded as emergency caesareans without labour and these had higher odds of neonatal mortality attributed to asphyxia, anoxia and trauma. Further research should focus on these unusual emergencies. Meanwhile for the vast majority of women these findings call into question the apparent ‘weekend effect’ identified in earlier analyses. They also show the strength of using large datasets which can be subdivided to identify a small subset which is not visible in analyses of smaller datasets.
This project, along with its predecessors, benefited greatly from methods of user involvement developed as part of the research, to involve maternity service users in research using linked anonymised administrative data.
The CHOICE Study was a NIHR-funded research project, led by the University of Edinburgh, investigating the safety, effectiveness, cost-effectiveness and acceptability of home cervical ripening during induction of labour (IOL). The process evaluation (qCHOICE) explored contextual influences on implementation of cervical ripening protocols and outcomes, women’s experiences of IOL and acceptability of home cervical ripening to women, their families, and other key stakeholders, and is being jointly conducted by City, University of London and University of Stirling. CHOICE began in December 2019, and completed in December 2022.
In addition to the main CHOICE study, qCHOICE team members have also undertaken two related projects: 1) a survey on the impact of COVID-19 on induction of labour practice in the UK; 2) and a feminist critical discourse analysis of induction of labour policy and guidelines in the UK.
Publications:
This NIHR-funded study of the feasibility and implications of conducting full-scale randomised controlled trial of an innovative method of induction of labour is now. Women who are booked for induction are randomised to receive either a prostaglandin pessary or a trans-cervical balloon catheter to start the induction of labour process. The aim was to compare how well these methods of labour induction work, which is the safest and least expensive method, and which is more acceptable to and favoured by women. The study found that a RCT is not feasible as there were insufficient numbers of pregnant women eligible and willing to participate in a trial. The nested qualitative study found that some women may prefer outpatient cervical ripening with a balloon catheter as they feel it enables them to stay closer to a spontaneous labour without use of drugs.
As part of this project, a systematic review was conducted of women’s experiences of induction of labour:
The main study results are reported here :
The rationale for this study derived from the reported low percentage of women having their babies in midwifery units (MU) despite the good evidence that suggests for women with uncomplicated pregnancies, having a baby in a MU results in better outcomes and is cheaper in comparison to having a baby on a traditional labour ward. Therefore, this study aimed to explore factors influencing the utilisation of midwifery units (MU) in England. Three articles on aspects of the findings were published.
Research group lead: Professor Susan Ayers
Our research focuses on the mental health and psychological wellbeing of mothers, their partners and children. Our work has three key areas: risk and resilience factors in perinatal mental health; assessment of perinatal mental health; and innovations in the delivery of perinatal mental health care and treatment.
This multidisciplinary group comprises 8 academic and research staff and 4 doctoral students working on projects ranging from national studies of mental health assessment to international studies of perinatal mental health. Current and recent research includes perinatal mental health in women in low and middle income countries; assessment of birth trauma and post-traumatic stress; evaluations of innovative interventions for perinatal mental health such as peer support interventions and development of local services.
We have established links with NHS Trusts and user-representative organisations in the UK, as well as international links with researchers in Europe, America, and Australasia. This includes the International Network for Perinatal PTSD Research, an international research initiative which is run by members of this group.
This study aims to identify the most effective, acceptable and feasible method for assessing anxiety in women during pregnancy and after birth. This will be achieved through 3 work packages (WP) that compare 4 different tools for assessing anxiety: 2 anxiety-specific measures and 2 mental health measures (GAD-7, SAAS, CORE-10, Whooley questions) selected on the basis of research and clinical evidence that suggest they may be effective. It will be conducted in NHS services in England and Scotland.
WP1 has been completed and currently finishing up analysis and writing up paper. WP2 recruitment was delayed due to COVID-19 however should be starting up in October 2020.
The MATRIx study is led by researchers at City, University of London in collaboration with experts across the UK. MATRIx reviewed the research evidence on what prevents women who are pregnant or after birth from getting support and treatment they need if they are struggling with emotional or psychological problems. On the basis of these reviews we developed recommendations for healthcare services about how to tackle these barriers to make sure women and families get the help they need. The project involved experts and stakeholders from many different backgrounds and disciplines.
Review 1 and 2 are now complete and two MATRIx conceptual frameworks were developed that highlight the importance of 66 barriers and 39 facilitators to perinatal mental healthcare at multiple levels that intersect across the care pathway. These conceptual frameworks informed the development of evidence-based recommendations on how to address barriers to ensure that all women are able to access the care and support they need. Recommendations were made for health policy, practice and research.
This is a mixed-methods qualitative study evaluating how risk is communicated and understood between healthcare professionals and pregnant women. Perception of risk in relation to pregnancy and childbirth is a complex and individual process influenced by multiple psychological and social factors. Women and health professionals may not recognise that others do not share their interpretations of risk and safety, which can lead to miscommunication and misunderstanding, and result in dissatisfaction and lack of engagement with healthcare.
To determine how women and healthcare professionals understand and communicate risk, we will be filming clinical consultations in antenatal clinics and analysing them through conversation analysis, as well as conducting interviews with women and healthcare professionals. Our findings will be used to create a communication tool to aid and improve conversations about risk in antenatal care. The study is being supervised by Professor Susan Ayers and Dr Suzanne Lee, and the research led by Dr Rebecca Webb.
This project aims to identify barriers to service improvement, and to inform and support effective solutions. Consequently, leading to good quality, evidence-based care pathways at the right time for all mums who need it. This project supports local leaders in four sites of England – Blackpool, Haringey, Southend and Gloucestershire, to improve the care and quality of life for mums with mental health problems during pregnancy and the first year of life, and their babies.
Caesareans performed late in labor, where the mother’s cervix is fully open and her baby’s head has entered her pelvis, can be complicated. If the baby’s head is deeply wedged in the woman’s pelvis, it can be difficult to lift it up to enable the baby to be born. This is called an impacted fetal head. There are a number of different techniques that can be used in this situation, however it is not clear which is the best or most effective. This project is looking at whether it would be possible to do a clinical trial to test these different techniques. The research team will conduct surveys and interviews with parents, obstetricians, anesthetists and midwives to gather their views and experiences of these births.
The first phase of interviews finished last year and a Delphi study has been completed (led by Nottingham). The project has been paused. City will conduct the second phase of qualitative work from October 2020 to Spring 2021.
This study involves a group of Australian researchers assisting women with depressive symptoms to increase their physical and mental wellbeing with physical activity.
This is a mixed methods study exploring first time mothers' and fathers' eperiences of fetal imaging (ultrasound and MRI) , and the effect it may have on the developing parent-fetal relationship. The project has received funding from the College of Radiographers and the Reseacrh Sustainability Fund at City, University of London and is a collaboration between two London universities; bringing together the work of the CMCHR at City, University of London and the Perinatal Imaging Department at King's College London. It is being conducted by doctoral study Emily Skelton, supervised by Prof.Susan Ayers, Dr.Christina Malamatenious and Prof.Mary Rutherford. Emily has completed a systematic review of twenty-three studies conducted by highlighted the important role of sonographers (healthcare professionals who perform ultrasound scans in pregnancy) in enhancing expectant parents’ experiences of scans through the provision of parent-centred care to facilitate the developing emotional connection between parents and their unborn babies. The review is published in the Journal of Reproductive and Infant Psychology.
This project started in September 2019 and has received verbal extension from funder to continue to November 2020, funded by Parent-Infant Foundation. Together with Baby is a parent-infant mental health service provided by Essex Partnership University Foundation Trust. We have been funded to evaluate the implementation of this service and answer the question - what factors enable and hinder its implementation? To answer this question, we are conducting a multi-method process evaluation, interviewing numerous stakeholders, clinicians providing the service and families receiving the service. We are also analysing quantitative data such as referral rates and intervention efficacy.
Project Lead at City: Dr Ellinor Olander
Project team members (including links to external partnerships): Dr Rose Coates, Dr Patricia Moran, Professor Susan Ayers
This collaboration with colleagues in Brazil looks at women’s perinatal mental health as part of the Birth in Brazil II Study of 20,000 women giving birth in Brazil. This study will help better understand risk factors, birth factors, and symptoms of depression, anxiety and PTSD in Brazilian women. This collaboration combines City’s expertise on perinatal mental health assessment, birth trauma, models of care and associated outcomes, with Brazilian expertise in perinatal epidemiology, evaluation and surveillance of public health interventions. It will improve understanding of perinatal mental health issues affecting women in Brazil and facilitate recognition and treatment of perinatal mental health problems.
Newton Links funding was obtained to extend the planned national survey to enable analysis of perinatal outcomes in relation to a range of factors in partnership with Fio Cruz research institute in Brazil. The extension also includes analysis by birth setting, with additional support from GCRF funds. The study was due to commence in March 2020 but the survey has been postponed because of the pandemic, although an initial planning workshop was completed. Ethics approval is in place with some minor amendments in process. Survey is expected to start now in October 2020, in one state at least, and if funded, will incorporate a large COVID analysis component
This project is a randomised controlled trial of testing for Group Streptococcus in pregnancy or intrapartum. It is funded by the NIHR HTA. The study has been currently paused due to COVID-19. However, a pre-qualitative study has been set up to understand knowledge on GBS-3 testing and views on implementing to inform the next study.
Research Group Lead: Dr Ellinor Olander
Our research focuses on population health, preventive action and health care for women and children including socially and economically marginalised groups, including issues of equity of access to and quality of care. We aim to describe inequalities in maternal and child health outcomes to inform public health policies and improve services for women, children and their families. Research includes young teenage parenting, mothering and feeding children with neurodisability, maternal and child health in relation to HIV/AIDS, and the health of homeless and migrant populations, obesity in pregnancy and in children, sickle cell and female genital mutilation. We are currently working on projects ranging from locally focussed studies in East London to national studies, such as on prevalence of FGM and the timing of birth and its outcome by time of day and day of the week and international comparisons of perinatal indicators. We use a range of methodological approaches including quantitative and qualitative methods and linkage and secondary analysis of national and linked datasets.
We have well established links with Barts Health NHS Trust, Homerton University Hospital NHS Trust and public health departments in East London as well as with the Department of Health, Home Office, the Office for National Statistics and non-governmental organisations such as Maternity Action and the NCT and international networks such as ROAM (Reproductive Outcomes and Migration) and Euro-Peristat. Our work has informed the development of maternal and child healthcare services and policy in England and internationally
This is a Horizon 2020 project funded by the European Commission to develop a systematic and in-depth understanding of acceptable, feasible and sustainable strategies to integrate group care into health systems for antenatal and postnatal care during the first 1000 days. Group care is evidence-based, transforms the delivery of maternal, new-born and child health care and reduces inequities in services utilization, improves the quality of services, and can make a positive impact on the health and wellbeing of mothers, families and children. It involves demonstration sites in 4 LMICs (Ghana, Suriname, South Africa, Kosovo), and 3 high-income countries (The Netherlands, Belgium, England) in settings that serve the most vulnerable women and girls. City is leading Work Package 5 on evaluation of the programme and has worked with two NHS maternity services to implement and evaluate innovative models of group care. In one setting, this is being combined with midwifery caseloading to enhance continuity and social support throughout the maternity period and in the other, midwives, health visitors and nursery nurses are collaborating across service boundaries to provide an integrated antenatal to postnatal model called Parenting Circles. This work builds on the work of the REACH Programme and the Pregnancy Circles trial (see Models of Care projects).
The study started in January 2020 but experienced delays and adaptations needed because of travel and social distancing restrictions affecting the care model. Evaluation data are currently being analysed with the aim of developing country implementation blueprints and an international implementation toolkit, to be published in 2024.
Midwife-Led Birth Settings (MLBS) available in the UK include homebirth services, alongside and freestanding birth centres. MLBS are associated with better clinical outcomes, better breastfeeding rates, lower risks of medium and long term morbidities, and high rates of experience satisfaction. However, existing evidence suggests that racialised women are less likely to access these services. The AMBeR Project aims to understand barriers and facilitators that impact access to MLBS for racialised individuals in the UK.
The study consists of five workstreams:
1. Scoping review: “Exploring existing literature around barriers, facilitators, and interventions related to accessibility of MLBS to racialised people in the UK”. Findings will be published soon. For further details, please see the review protocol here.
2. Surveys of UK midwives: We are conducting a survey via the UK Midwifery Study System (UKMidSS) network of midwifery units to identify current or past strategies, initiatives and interventions designed to increase the accessibility of birth centres. Another survey related to homebirth services is being planned in collaboration with the Royal College of Midwives (RCM).
3. Qualitative interviews with midwives: Interviews with a sub-sample of survey respondents and key informants will be conducted to obtain further detail on reported interventions and explore perceptions of the barriers and opportunities in terms of accessibility of services to racialised service users.
4. Analysis of routine MSDS data: We are planning to conduct quantitative analysis of routine data from the NHS Maternity Services Data Set to explore maternity service use by ethnicity.
5. Last but not least, we are planning knowledge exchange activities with the community to discuss our emerging findings and gather thoughts for potential next steps for co-produced research around this topic.

This was an observational feasibility study with a nested qualitative study to assess whether it is feasible and acceptable to screen an at-risk migrant population for LTBI at routine antenatal booking visits in secondary care, using opt-out IGRA testing. Secondly, to develop a definitive large-scale cluster RCT to evaluate the effectiveness of acceptable interventions to maximise migrant screening for LTBI in pregnancy and to increase uptake of treatment postpartum. Pregnant migrants from high TB-incidence countries will be recruited, collecting data using interviews and focus groups of migrants and LTBI knowledge questionnaires.
This study has now been completed and reports are in submission. The protocol was published here:
This is a qualitative study involving interviews with healthcare professionals to understand their experiences of working with young mothers. Furthermore, with young mothers to understand their experiences in eating and moving during and after pregnancy.
This a co-design study, involving 3 groups of people – carers, healthcare professionals and young people, looking at different interventions of sickle cell anaemia. The aim is to develop an intervention to enhance and improve health care provision of sickle cell anaemia.
The general objective is to understand the relationship between medical teams in maternity services and people (users) with a non-western cosmology. The project will illuminate this issue through cross- cultural comparison. In the Brazilian context the focus is on the encounters of indigenous women with health services, while in the UK the focus will be on those of refugees and recent immigrants. A same question will constitute the background of these two studies: how public health policies can account for the cultural diversity in a way that provide adequate care without disrespecting other world logics? The Brazilian part of the research will essentially consist in data analysis of an almost already completed fieldwork, while the UK part will give rise to rapid ethnographic case studies, supplemented by bibliographic and documentary data.
This study aims to improve the way that positive newborn screening results for conditions such as sickle cell disease and cystic fibrosis are communicated to parents by health professionals. With the expansion of newborn screening in England, the importance of delivering screening results appropriately to minimize any long-term negative health and psychological consequences is vital; this project aims to develop interventions to improve such communication. It involves four phases and as a part of the project, the researchers will work with parent representatives for each screened condition covered by newborn screening who will form an advisory group to assist the research team, provide feedback on each phase of the project and monitor its progress.
This project was paused between March and July 2020 and has now resumed properly from September 2020 and will be finishing in December 2020.
This study will evaluate child nursing student views and experiences on peer mentoring and understanding how to train them as peer mentors, in addition to assisting them in mentoring other colleagues as well.
This study involves interviewing young people, carers and parents of those diagnosed with sickle cell anaemia to assist in the development of an educational pack for student nurses. This pack should include all necessary information of what a student nurse should know in regards to this illness.
Research Group Lead: Dr Susan Bradley
A developing strand of our work is addressing quality of MCH care globally, including in low and middle-income countries. This strand builds on a series of doctoral projects addressing subjects as diverse as HIV, female genital mutilation, health system stewardship, maternal health and respectful maternity care. Our work is now focused on the implementation of high quality and respectful care, goals that are now reflected in World Health Organisation policies and in the Sustainable Development Goals. We explore how structural factors and the organisation and models of care can influence maternal and child health and wellbeing, positively or negatively. We are focused on translation of international evidence on the value of midwife-led care in a range of contexts. Aspects of our work also bring lessons for improving maternal health and care from low-income countries to higher income settings like the UK, through community-based interventions and women’s groups – for example in models such as group care (see projects).
Recent support from the Global Challenge Research Fund has enabled us to:
We draw on critical realist approaches, post-colonial and de-colonising theories to provide a critical analysis of the forces influencing quality, safety and experience of care, including cultural safety. We also use implementation science theory to inform our thinking about how to implement change, but with a strong focus on social and structural approaches which take into account the
This is a Horizon 2020 project funded by the European Commission. It aims to develop a systematic and in-depth understanding of acceptable, feasible and sustainable strategies to integrate group care into health systems for antenatal and postnatal care during the first 1000 days. Group care is evidence-based, transforms the delivery of maternal, new-born and child health care and reduces inequities in services utilization, improves the quality of services, and can make a positive impact on the health and wellbeing of mothers, families and children. It will use demonstration sites in 4 LMICs (Ghana, Suriname, South Africa, Kosovo), and 3 high-income countries (The Netherlands, Belgium, UK) in settings that serve the most vulnerable women and girls, will deliver group antenatal and postnatal care throughout the project.
Specifically, GC_1000 will:
1. Implement group antenatal and postnatal care in selected demonstration sites in collaborative ways that set the groundwork for sustained service delivery and possibilities for scaling- up;
2. Analyse within country data that emerge from the implementation process to create country-specific blueprints for scale-up;
3. Use cross-country synthesis to develop a global implementation strategy toolbox for the adaptation, implementation and scale up of facilitated group care within the first 1000 days, particularly to reach the most vulnerable groups of women and girls globally.
This study started in January 2020. This study is experiencing some delays and adaptations needed because of travel and social distancing restrictions affecting the care model directly but there has been work on adaptations to the model and methods of initial data collection to compensate for this. City is leading Work Package 5 on evaluation of the programme.
This is an on-going research and development programme to test whether the introduction of midwifery units (MUs), staffed by dedicated midwives, can improve the birth environment and experience of care for women and midwives in low- and middle-income countries (LMIC). IMaGINE focuses on the potential of midwifery-led care and services to address the complex, multi-faceted problems of widespread disrespect and abuse during birth, lack of evidence-based practice, and women’s reluctance to engage with facility-based birth. While we have robust evidence from high-income countries on the benefits of midwife-led care models (for women and midwives), such evidence is lacking from resource-constrained contexts. The initial stages of our programme were supported by Global Challenge Research Funding. This enabled us to establish a network of actors from Malawi, Sudan, Brazil and India and to work together to carry out a systematic review/ meta-synthesis of current evidence on the impact of midwifery units in LMICs. We have also undertaken key stakeholder workshops and situational analyses in three of the four partner countries. Future plans involve identifying pilot project sites to carry out implementation and evaluation of MUs in these contexts.
The project has progressed, with planned work completed in Brazil, Malawi and Sudan and but the work in India had had to be postponed because of the lockdowns and travel restrictions.
This is an ethnographic study, exploring the complexity of social processes on decision-making related to the universe of meanings, reasons, beliefs, values and attitudes that influence women’s birthplace choice.
This project involves collaboration with colleagues at the Oswaldo Cruz Foundation (Fiocruz) in Brazil. It is forms part of a wider study to look at women’s perinatal mental health as part of the Birth in Brazil II Study of 20,000 women giving birth in Brazil. This study, funded by the Newton Fund, will help better understand risk factors, birth and care factors, and symptoms of depression, anxiety and PTSD in Brazilian women. The Birthplace in Brazil study, funded by the Grand Challenges Research Fund enables us to look specifically at outcomes of births planned in freestanding midwifery units in Brazil. Development of midwifery units (Centros de Parto Normal) formed a key part of the maternity reform policy in Brazil, to improve outcomes and experiences of care and reduce the excessive rates of intervention. However, only a small number have been implemented to date and these are mainly concentrated in a few cities. This study will help to provide evidence which should increase confidence in implementation across Brazil.
Researchers at City: Dr Nathalie Leister, Dr. Rose Coates, Dr. Louise Williams, Prof. Christine McCourt, Prof. Susan Ayers
Partners: Friocruz, Brazil
City, University of London has formed a partnership with a Brazilian institution. This project is exploring maternity care in Brazil including a national survey of obstetric units, midwifery units and surveying over 20000 women.
This study explored midwives’ perspectives on the practice, impact and challenges of delivering respectful maternity care in Malawi, highlighting the considerable challenges facing staff in this context. Prior to this, much of the research had focussed on women’s experiences. This work aimed to include the voice of the midwife.
Two systematic reviews were conducted to understand the broader drivers of disrespectful care during birth in sub-Saharan Africa. One explored women’s experiences; the second focussed on midwives perspectives.
This study aims to show the optimum maternal and perinatal outcomes in Midwifery Units, explore the reasons for why majority of women with uncomplicated pregnancies give birth in obstetric units when there is no clinical indication and the reasons behind choosing this environment against the evidences on places of birth.
Research Group Lead: Dr Lucia Rocca-Ihenacho
The Midwifery Units (MU) Standards were developed by a team led by Dr Rocca-Ihenacho as part of her NIHR Knowledge Mobilisation Fellowship, thus being translational. The aim of the standards was to support the implementationof the evidence produced by our prior research on place of birth and particularly to support maternity units planning to open new MUs or improving existing ones.
The MU Standards were launched during the second MUNet Conference at City in July 2018 and we now want to develop indicators and an assessment tool in order to further develop impact. The Standards document includes 27 standards under 10 themes that capture the evidence base, translating it into more practical guidance. At present the Standards do not include indicators for users to benchmark where their service is in relation to the Standards or any improvements achieved. The number of indicators is expected to be approximately 50.
We propose to create indicators and a self-assessment tool for users to assess their own services against each of the published Standards. This can also hold future income generating opportunities for MUNet in terms of creating an accreditation system.
The aim of this study is to develop and evaluate a theoretically informed knowledge implementation pathway that service providers and commissioners can use as a guide to implement evidence on birthplace into NHS services which require complex organisational and professional practice change.
This study has been completed and is in the analysis stage.
Barkantine report
As the Research for Equitable Antenatal Care and Health (REACH) Pregnancy Circles trial was drawing to a close in 2020, a team of researchers from the Centre for Maternal and Infant Health Research at City were granted funding for a small study exploring how this innovative model of group antenatal care might be rolled as part of normal NHS maternity care.
In order to better understand midwives’ lived experience of facilitating gANC within the NHS, it was felt that practising midwives should be involved not only as participants, but as partners in the study design, data collection and analysis alongside the research team. A co-production framework was employed, adapted from Henshall et al (2018) and three midwives from different Trusts who had facilitated Pregnancy Circles were recruited to collaborate. The midwives contributed to the topic guide and took the lead in facilitating the online focus group discussion with their peers. Different aspects of the data were then analysed by each member of the team, with findings summarised and discussed together. The partnership has proved to be a rich source of discussion and insight, balancing theoretical insight with practical realities.
Findings are currently being written up for a journal article.

Professor Susan Ayers

Dr Katherine Curtis-Tyler
The Centre hosts research seminars regularly as part of the School of Health and Psychological Sciences’ weekly research seminar programme. All are welcome to attend but it is essential to contact the organiser beforehand for room and catering planning and in case of any late changes or cancellation. We will aim to make presentations or podcasts available on the website where possible.
Check back for details of future events.

Part 1:
Part 2:



The Society for Reproductive and Infant Psychology (SRIP) is an international organisation bringing together research on psychological, socio-cultural and political aspects of reproduction, birth and infancy. The Society raises awareness of psychological, social and political aspects of reproductive and infant health through scientific conferences and workshops, our journal The Journal of Reproductive & Infant Psychology, and liaising with professional bodies and the public.
Our annual conferences provides the means to exchange research findings, develop research interests, develop research networks and engage with clinical and academic partners.
At the conference, Dr Lucia Rocca-Ihenacho and colleagues launched the Midwifery Unit Standards developed as part of an NIHR post-doctoral fellowship at City, University of London. The Standards have been developed over an 18 month period by a team of researchers with input from a broad range of stakeholders across the UK and mainland Europe, RCM, EMA and delegates at the 2017 ICM conference.
They celebrated Birth Centre Beacon Sites and certificates were presented by Kathryn Gutteridge, President of the Royal College of Midwives.
Leading midwives and policymakers from all four countries of the UK presented on making services more responsive to women's and babies' needs, more family-friendly, and unlocking the potential of birth centres.
Sessions:
This conference aimed to share research and experiences related to positive birth. Featuring a number of high profile speakers and guests from the area, the day shared some of the latest research from the discipline as well as service users’ experiences in order to explore the concepts of positive birth and informed choice. The event was organised by Judith Flood, a midwifery lecturer in the School of Health and Psychological Sciences at City.
Student nurses and midwives showing strength in support of NHS
Recommendations for how midwifery units can support the NHS during COVID-19 crisis
Improved access to Midwifery Units is urgently needed
How do we best measure the effect of PTSD on women following traumatic childbirth?
City pregnancy programme shortlisted for Royal College of Midwives innovation award
In collaboration with the Royal College of Midwives, the Midwifery Unit Network offers support to those wishing to develop midwifery units (birth centres), and to already established midwifery units. The network acts as a hub to share good practice and information resources, and be a community of practice with a shared philosophy essential to offer consistent, excellent and safe care for women and their families.
The aim of the Midwifery Unit Network is to maximise potential for a positive childbirth experience, and to enhance the physical and psychological wellbeing of childbearing women and their babies, through the promotion and support of midwifery units (birth centres).
This is a network of researchers and clinicians who are working together to reduce birth trauma and perinatal PTSD across the world.
The website provides information on the latest perinatal PTSD research, events, and an interactive blog where researchers can interact and post questions. The latest research papers on perinatal PTSD are posted monthly.
The Centre runs a Patient and Public Involvement group where parents and parents-to-be collaborate on research projects. To date, parents have helped develop questionnaires, participant recruitment strategies and grant proposals.
We have a range of questionnaires and research tools that are freely available to download or use on request. These include:
City Infant Faces is a database of standardised photographs of baby faces showing different emotions. These have been categorised into positive, negative and neutral emotions and can be used in studies of the perception of infant emotions. The City Infant Faces database has been validated and is available on request for research use only (contact us).
The CityBiTS is a questionnaire measure of post-traumatic stress disorder (PTSD) after birth. This questionnaire measures symptoms and diagnosis of PTSD according to DSM-5 diagnostic criteria. It also includes items from DSM-4 that research suggests are discriminative when diagnosing postnatal PTSD. Available on request (contact us).
The CityMISS is a questionnaire measure of perceived stigma for mental illness in pregnancy and postpartum. It is available on request (contact us).
The SCIB measures control during birth and perceived support from health professionals. It has 3 subscales: support from healthcare professionals, perceived internal control, and perceived external control. Validated versions are available in English, German and Turkish:
SCIB – English version
SCIB – German version
SCIB – Turkish version
The P-BESS measures experiences and satisfaction with care during the birth of a preterm baby. It can be used with mothers and fathers. Validated versions are available to download in English. A Portuguese version is currently being validated so will be available soon.
P-BESS English version
The BirthMARQ measures women’s memories of birth and aspects of recall. It has 5 subscales of: (1) emotional memories, (2) centrality of memories to self, (3) coherence of memories, (4) reliving of memories and (5) recall of memories. Validated versions are available to download in English. Persian and Czech versions are currently being validated so will be available soon.
BirthMARQ